
Over 90% of Corporate Directors at Canada’s Biggest For-Profit Nursing Homes Have No Medical Qualifications
Corporate boards of directors at Canada’s four biggest for-profit nursing home chains are dominated by real estate developers
Despite holding life-and-death decision-making power over tens of thousands of elderly Canadians, the country’s biggest for-profit nursing home chains are largely dominated by corporate directors with no real medical expertise.
To date, 85% of Canada’s COVID-19 deaths are linked to outbreaks at long-term care facilities, with private, for-profit homes seeing up to four times as many deaths.
But according to a new analysis of corporate records by PressProgress looking at 35 directors currently sitting on the boards of Canada’s four largest for-profit nursing home chains, including Sienna Living, Extendicare Inc., Revera and Chartwell, most have little to no expertise on matters relating to providing care.
In total, 40% of the directors sitting on the boards of these for-profit nursing home chains have backgrounds in real estate.
17% of corporate directors hold executive positions in finance while another 17% hail from other corporate sectors, like hospitality, insurance or energy.
14% held positions in private health services or pharmaceutical companies, however, only three board members out of the 35 board directors (9%) are identified as certified healthcare professionals.
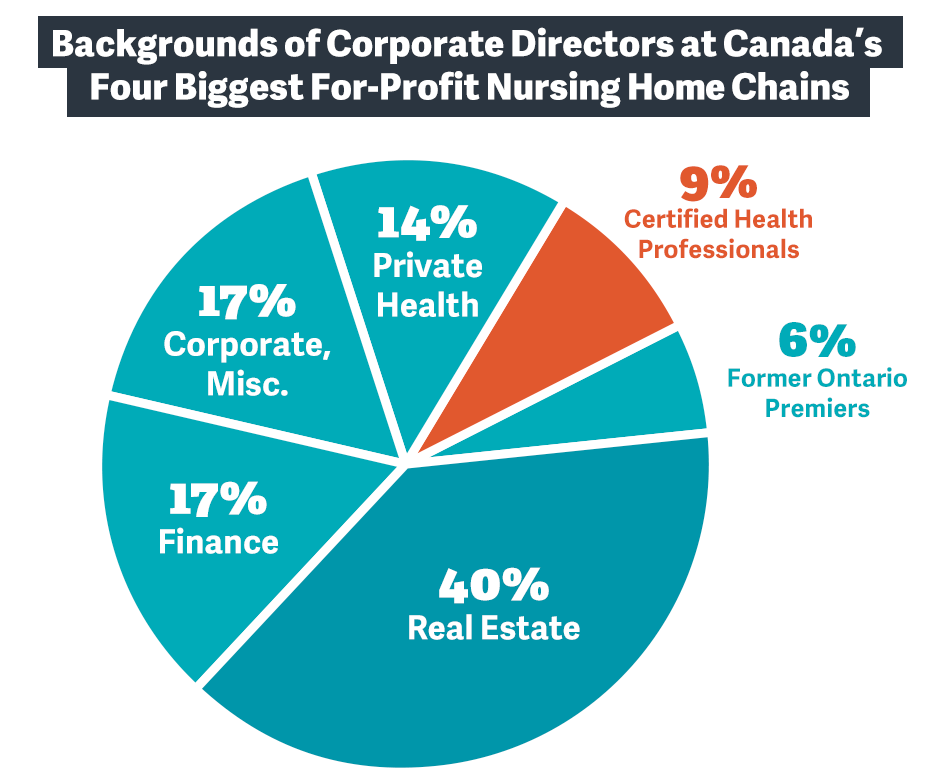
Graphic: PressProgress
In fact, two companies — Chartwell and Sienna — do not currently have any certified healthcare professionals sitting as board members.
All four companies did not respond to questions from PressProgress about the compositions of their boards of directors.
According to shareholder reports and corporate profiles reviewed by PressProgress, the four companies alone operate nearly 80,000 beds and units across Canada. In 2017, an international study found those companies own more than one-fifth of all nursing home beds in Canada.
Jacqueline A. Choiniere, a nursing professor at York University who co-authored a recent CCPA report on long-term care, told PressProgress the board compositions are a reflection of deep problems with the for-profit long-term care model.
“We’ve treated this sector as housing stock,” she said. “We need focus to where it needs to be, which is on the care that has to occur within that sector. We need to get away from this for-profit delivery of care in that sector.”
Choiniere said the for-profit delivery model negatively impacts working conditions and quality of service.
“The ownership model emphasizes the wrong principles,” Choiniere explained. “We see private-sector managerial practices being applied. That means more casual part-time staff, that means an emphasis on efficiency when it comes to staffing, that means contracting out food and housekeeping.”
In particular, the CCPA report notes the tendency of for-profit nursing home chains to contract out services “brings even more people into the home on a daily basis, people who can present a risk and be at risk.”
The nursing home industry’s increasing reliance on casual and part-time labour also presents other health risks:
“Especially given the low wages and benefits, most of these part-time and casual workers want and need full-time work. As a result, they take another part-time job at another care home, travelling there by public transit because few can afford a car. The risk of sharing any virus is obvious.”
Melanie Benard, National Director of Policy and Advocacy with the Canadian Health Coalition, said board members of long-term care home chains should have the qualifications needed to ensure the quality of the service they provide.
“In for-profit facilities, there’s an underlying conflict between investing in resident care and increasing shareholders’ profits,” Benard said. “We’re trusting these people to care for some of the most vulnerable members of our society.”
“Long-term care shouldn’t just be seen as a real estate or business investment.”
Facilities owned by private companies are currently experiencing some of the most deadly COVID-19 outbreaks in Canada.
Data compiled by journalist Nora Loreto has identified over 5,000 COVID-19 deaths linked to long-term care homes as of late May.
A recent analysis by the Toronto Star found that residents in Ontario’s for-profit homes are about twice as likely to catch and die from COVID-19 as those in non-profit homes, and about four times as likely to become infected and die from the disease as those in municipal homes.
Families of residents at facilities owned by Sienna and Revera recently launched a class-action lawsuit alleging negligence and breach of contract over the companies’ handling of outbreaks at facilities in Ontario.
“I believe that a lot of the residents were infected with COVID because the proper infection controls weren’t being used or followed proper procedures,” one family-member told CBC.
Revera alsofaces a class-action lawsuit from families of residents at a facility in Calgary.
In a public statement, last month, Revera said: “Our homes regularly meet or exceed government standards, and we have been following government directives since the outset of the pandemic. We have also been working closely with government partners as the pandemic has progressed.”
Chartwell is also being sued over its handling of coronavirus outbreaks at its facilities. Earlier this month, the family of an Ontario woman who died from COVID-19 at a Chartwell residence launched a class-action lawsuit alleging the long-term care provider’s failure to properly respond to the pandemic caused “preventable deaths and unnecessary suffering.”
Former Conservative Ontario premier Mike Harris serves as Chair of Chartwell, while former premier Bill Davis is chair emeritus of Revera.
Our journalism is powered by readers like you.
We’re an award-winning non-profit news organization that covers topics like social and economic inequality, big business and labour, and right-wing extremism.
Help us build so we can bring to light stories that don’t get the attention they deserve from Canada’s big corporate media outlets.
Donate



