
New Study Shows BC’s Access to Safe Supply is Saving Thousands of Lives
New study published in the British Medical Journal shows mortality rates among people prescribed safe supply were 61% lower
Despite efforts by right-wing media, politicians and recovery industry advocates to undermine the validity of prescribed safer supply, a new BC-based study has demonstrated improved health outcomes and reduced risk for recipients of safer supply.
The study, which was published in the British Medical Journal, surveyed over 5,000 people with opioid use disorders who were prescribed more than a one day supply of opioids were 61% less likely to die the following week compared to a similar group of people who did not receive a prescription.
New study: People with an opioid use disorder prescribed 1+ day’s supply of opioids as part of BC’s Risk Mitigation Guidance were 61% less likely to die in the following week, compared to a similar group of people who did not receive a prescription. https://t.co/NsxUT3nMNu pic.twitter.com/PaaQp7ATFq
— BC Centre for Disease Control (@CDCofBC) January 11, 2024
The timeline of the study was from 2020 to 2021, when the province of British Columbia issued “Risk Mitigation Guidance,” which allowed doctors to prescribe opioids and stimulants to people at risk of overdose, withdrawal or other drug related harms.
Dr. Amanda Slaunwhite, the first author of the study and a senior scientist at BCCDC, as well as an assistant professor in the UBC School of Population & Public Health, says the study was intended to compare outcomes among people who received the prescription (of safer supply) to people who did not receive the prescription.
“This study really provides foundational research evidence that providing pharmaceutical alternative opioids in the context of a provincial public health emergency where we have an extremely toxic illicit drug supply that is killing seven people per day, can potentially reduce deaths among people with opioid use disorder,” Dr. Slaunwhite told PressProgress.
“That is a really significant finding. It shows that the guidance that was issued in March 2020, did have a positive impact, it did reduce deaths among the people who received the medication. And that is a really encouraging finding for the clinicians.”
Dr. Slaunwhite says that while more research is needed, she hopes that the discoveries made are used to inform interventions into the ongoing crisis in BC and across Canada.
“There’s a significant need to reduce mortality among people who are using drugs. So my hope is that this research is used to further develop and inform how we design interventions to address the toxic drug crisis, which is very multifaceted and requires many different types of interventions across the continuum of care to address.”
The BMJ also published an associated editorial authored by researchers, academics and physicians across the UK and Canada based on the research study.
Dr. Tommy Brothers, a clinician, doctor and researcher in Halifax, Nova Scotia, and one of the authors of the editorial, says that while there is always going to be a need for more research, interventions that have been proven to have a positive impact should not be withheld.
“This is supporting and confirming the evidence that already existed and going beyond it to say with even more confidence that on average, this is a beneficial intervention that we should make more widely available,” Dr. Brothers told PressProgress.
“The problem underlying the horrendous, catastrophic number of overdose deaths is the toxicity of the drug supply.”
Dr. Brothers says that it is clear when looking at the data, that places with a more toxic drug supply have a higher rate of overdose death, and that safer supply could make a clear impact.
“The evidence is clear that a safer drug supply is less risky, and that places that have a safer drug supply, there’s less deaths. Across Canada, where I am in Atlantic Canada, if you look at those Health Canada heat maps—BC is dark purple, Alberta is dark purple, but here we are in Atlantic Canada, we’re like light gray. And the reason is that we still have predominantly pharmaceutical opioids in our street drug supply,” Dr. Brothers added.
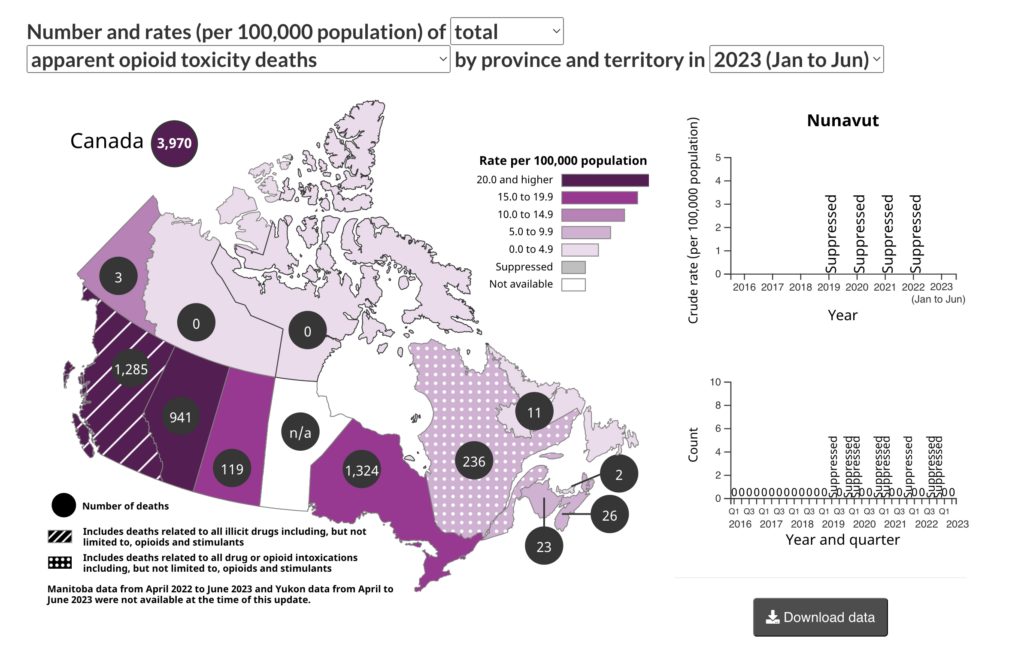
Health Canada Map of Overdose Crisis
While op-eds in right-wing media outlets like the National Post have attempted to drum up anxieties around the diversion of safe supply, Dr. Brothers says the positive health impact could only be observed if those who were prescribed the safe supply were the ones actually using it.
“The fact that people who were prescribed the medication had a mortality benefit means that they have to have been taking it. Like these would have been the highest risk people who are dependent on unregulated fentanyl, and they’re getting these pharmaceutical prescriptions, and then they’re dying less often,” Dr. Brothers said.
“It means that they would have had to be taking that safer supply medication not not selling it all for fentanyl.”
Against the backdrop of the moral panic, Dr. Brothers says the evidence should speak for itself.
“Things are at the point now, and as we tried to say in the editorial, that we shouldn’t delay its roll-out further,” Dr. Brothers said. “There’s enough convincing evidence now that the problem is the toxic drug supply, and a fundamental solution is intervening on that by providing safer alternatives. And then we need to continue to evaluate and do research, but not withhold the intervention.
“Nothing is just scientific. It’s all moral and political as well.”
Our journalism is powered by readers like you.
We’re an award-winning non-profit news organization that covers topics like social and economic inequality, big business and labour, and right-wing extremism.
Help us build so we can bring to light stories that don’t get the attention they deserve from Canada’s big corporate media outlets.
Donate



